Scarring alopecia is a severe form of hair loss. The body’s inflammatory cells attack the follicles and replace them with scar tissue. This creates smooth, bald areas where hair cannot regrow.
There are several forms of scarring hair loss. These include frontal fibrosing alopecia, lichen planopilaris, and central centrifugal cicatricial alopecia.
Permanent loss is devastating, yet early diagnosis offers hope. Proper diagnosis and management can halt the destruction of follicles. The key is prompt intervention before too many follicles are lost. Delay can lead to irreversible loss.
The Cosmedica Clinic, one of the most renowned hair transplant clinics in Turkey, has achieved strong outcomes with early diagnosis of scarring hair loss. They combine advanced medical therapies with surgical techniques like direct hair implantation (DHI).
These techniques can restore hair to bald areas. Below, we outline the main types of scarring hair loss and the diagnostic process. We also review current treatments.
Non-Scarring vs. Scarring Alopecia
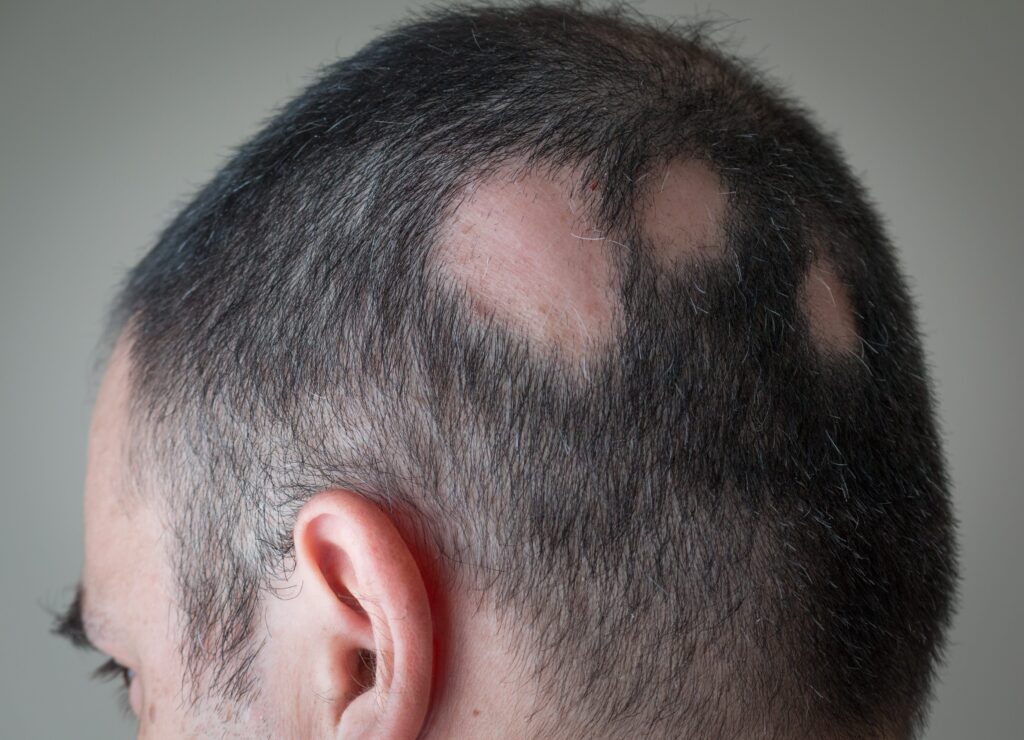
Alopecia means hair loss. In non-scarring alopecia, hair follicles are not permanently damaged. With proper care, hair can regrow. Common types include:
- Male/female pattern hair loss (androgenetic alopecia)
- Alopecia areata
- Telogen effluvium
- Traction alopecia
Scarring alopecia involves permanent follicle destruction due to inflammation and scar tissue. The follicle itself is the target. Inflammatory cells replace it with scar, making future growth impossible. About 3% of dermatology cases involve this type of loss.
What Are the Different Types of Scarring Alopecia?
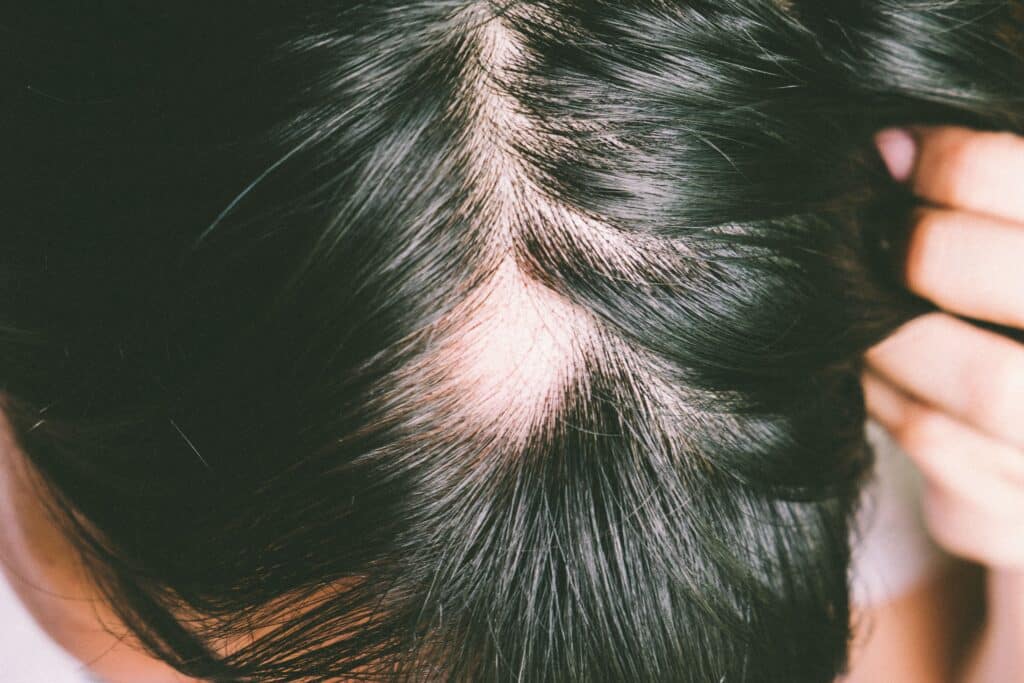
Scarring alopecias are primary or secondary. Main primary (“cicatricial”) types:
Central Centrifugal Cicatricial Alopecia (CCCA)
CCCA is more common among Black women and women of African descent. It starts at the crown and spreads outward in a circle. Ongoing inflammation and scarring can cause permanent loss.
Frontal Fibrosing Alopecia
FFA is the most common scarring hair loss. It occurs in about 10% of hair loss cases. It scars the frontal hairline, eyebrows, and sometimes body hair.
Lichen Planopilaris (LPP)
LPP is a chronic inflammatory disease. It causes patchy loss, often on the sides and back. Lymphocytic cells attack follicles and leave scar tissue.
Folliculitis Decalvans
This is a neutrophilic inflammatory condition. It causes swollen, pus-filled spots and later scarring hair loss.
Dissecting Cellulitis
This condition can form abscesses, cause scarring alopecia, and may have systemic symptoms.
Lupus Erythematosus
Chronic cutaneous lupus erythematosus is an autoimmune disease. The body attacks its own tissues, including hair follicles. This can cause scarring and permanent loss.
How Scarring Alopecia Is Diagnosed
Diagnosis starts with a detailed history. Your doctor will ask when shedding began, how it spread, and what triggers flares. They will review hair care, styling, and past treatments. They will also screen for autoimmune symptoms.
Next comes a careful scalp exam. Doctors look for redness, scaling, pustules, and shiny patches. They often use dermoscopy to view follicles in high detail. Photos help track change over time.
Basic tests may rule out other causes. Blood work can check general health when indicated. A scalp biopsy is the key step in many cases. It is taken from the active edge of a lesion.
The sample is reviewed under the microscope. Patterns of inflammation point to the type of scarring alopecia. This guides drug choice and the intensity of care. It also sets expectations for regrowth near affected zones.
Monitoring matters as much as the first visit. Follow-ups every few months check for new activity. If signs calm and remain quiet, maintenance can begin. Clear documentation helps decide when surgery is safe to consider.
What Does Scarring Alopecia Look Like?
Early, active disease shows patches of loss with:
- Redness and inflammation
- Scaling, flaking, or peeling
- Pustules (pus-filled spots)
- Itching, burning, or pain
- Crusting or oozing lesions
As inflammation progresses, more follicles are destroyed. Small bald patches merge into larger shiny areas. Scar tissue prevents regrowth.
Patterns vary by type. CCCA affects the crown and spreads outward. Lichen planopilaris favors the sides and back. FFA causes a receding frontotemporal hairline.
Research Insights and Related Conditions
Researchers are focusing on stem cells in the follicle bulge, the long-lived cells that enable normal regrowth. When inflammation wipes out these stem cells, the follicle loses its ability to repair. That loss explains why scarring alopecia is permanent.
The health of sebaceous glands also matters. These oil-producing structures support the follicle and help modulate local inflammation. Damage to sebaceous glands can destabilize the unit and accelerate scarring.
Patterns vary across groups, and many affected women present with frontal fibrosing alopecia or central centrifugal cicatricial alopecia. Eyebrow thinning or crown-centered loss are common early clues. Autoimmune overlap is another driver, as discoid lupus erythematosus can scar the scalp and leave pale, moth-eaten patches. Recognizing these signals steers therapy before more follicles are lost.
Infections and mechanical stress contribute as well. Acne keloidalis at the nape can create firm papules and plaques that foster chronic inflammation and secondary scarring if untreated. Early anti-inflammatory care, gentle hair practices, and sun protection help preserve the remaining follicle niche.
Can Hair Grow Back with Scarring Alopecia?

Unfortunately, scarring hair loss is permanent. Destroyed follicles cannot regrow hair. Early diagnosis and strong treatment are crucial. Doctors use scalp biopsy and lab tests to confirm the cause.
The goal is to stop progression before more follicles are lost. Scarred follicles remain permanently bald.
Treatment Plan, Timeline, and Expectations
Treatment comes in phases. First, calm the inflammation quickly. Doctors may use topical steroids, intralesional steroids, or oral agents. Some patients also receive antibiotics with anti-inflammatory effects.
The next phase is stabilization. Visits every 8–12 weeks assess symptoms and photos. If flares persist, the plan is adjusted. Added options can include hydroxychloroquine, immunosuppressants, or PRP.
Supportive care protects remaining follicles. Minoxidil can aid surrounding hair. Gentle cleansing reduces scale and irritation. Sun protection and low-tension styling reduce triggers.
Expect months, not weeks, for control. Many plans run six to twelve months before tapering. Once the disease is quiet, surgery may be discussed. Surgeons prefer a stable scalp for at least a year.
Transplant goals must be realistic. Scar tissue limits blood flow and density. DHI or FUE can still improve framing and coverage. Sometimes surgeons pair grafts with SMP for fullness.
Regular follow-up keeps gains on track. Report new redness, pain, or pustules early. A steady, staged plan offers the best long-term results.
What are the Treatments for Scarring Alopecia?
Treatment aims to calm inflammation and prevent further permanent loss. Typical options include:
Antibiotics and Anti-Inflammatories
Oral antibiotics like doxycycline or minocycline can reduce infection and inflammation. Topical corticosteroids applied to affected areas also help.
Steroid Injections
Doctors inject corticosteroids such as triamcinolone into the scalp. This targets local inflammation.
Immunosuppressants
Severe autoimmune disease may need immunosuppressants. These drugs quiet an overactive immune system. They are useful in conditions like lupus erythematosus.
Immunomodulators
Hydroxychloroquine can shift the immune response away from the follicles.
Hair Growth Stimulation
Minoxidil and platelet-rich plasma (PRP) may support growth around affected areas.
Hair Transplantation
Transplants can restore hair to stable, scarred areas. Surgeons use follicular unit extraction (FUE) or the DHI technique. You can look the different options and at the price of a hair transplant in Turkey at Cosmedica Clinic to help you choose your desired procedure.
Conclusion
Scarring hair loss is hard to face. Watching hair thin and vanish is disheartening.
Act quickly if you see redness, scaling, or new bald patches. Scarred follicles will not recover.
Treatment can stop further destruction. Be proactive and consider every option. A comprehensive plan can reduce visible impact. You can always head over to Cosmedica Clinic for a free hair consultation and evaluation.
FAQ
What is scarring alopecia and how does it differ from non-scarring alopecia?
Scarring alopecia involves the permanent destruction of hair follicles due to inflammation and scar tissue, preventing regrowth. In contrast, non-scarring alopecia allows for hair to regrow as the follicles remain intact and functional.
What types of scarring alopecia exist?
Common forms of scarring alopecia include Central Centrifugal Cicatricial Alopecia, Frontal Fibrosing Alopecia, and Lichen Planopilaris. Each type has unique characteristics, such as location and pattern of hair loss on the scalp.
Can hair ever grow back after scarring alopecia?
No, hair cannot regrow once follicles are scarred and destroyed in scarring alopecia. Early diagnosis and treatment are essential to prevent further follicle damage, but once scarring occurs, those follicles remain permanently bald.
What treatment options are available for scarring alopecia?
Treatment focuses on preventing further hair loss and calming inflammation. Options include antibiotics, steroid injections, immunosuppressants, hair growth stimulators, and possibly hair transplants, such as DHI, offered at specialized clinics.
